Contact number: 020 7806 4060
What Are Kyphoplasty and Vertebroplasty?
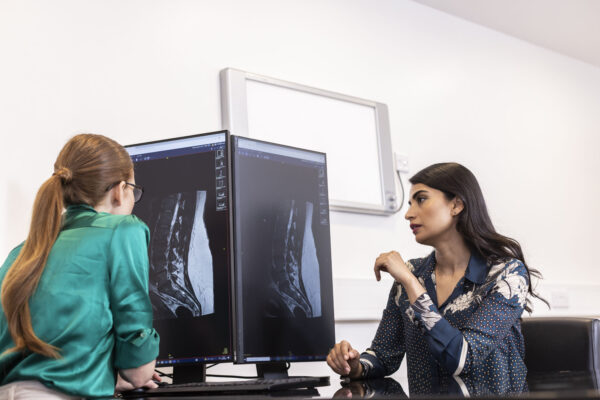
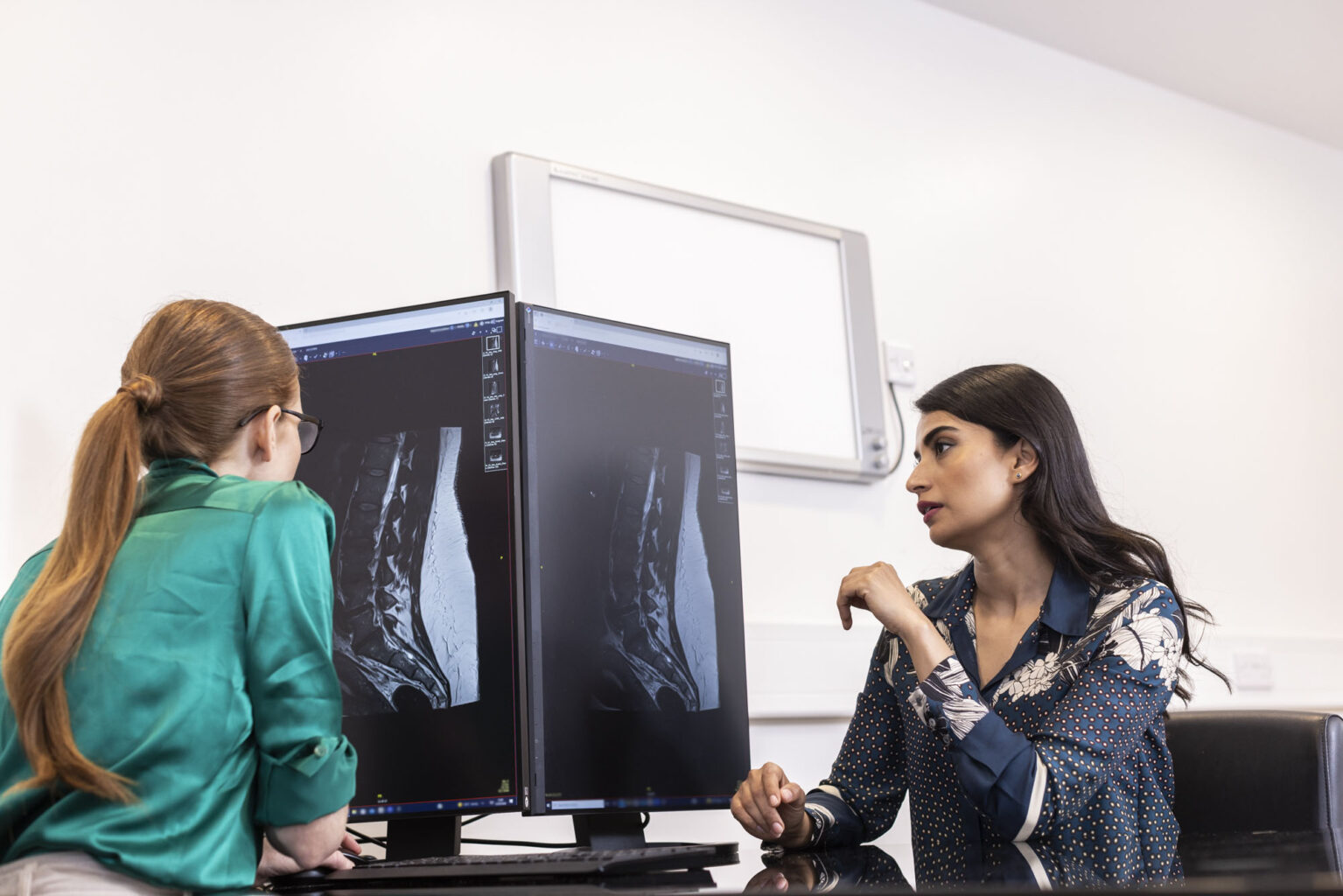
Kyphoplasty and vertebroplasty are procedures that stabilise fractured vertebrae by injecting medical-grade bone cement into the damaged area. These treatments are particularly effective for compression fractures caused by weakened bones.
- Kyphoplasty: Involves inflating a small balloon inside the vertebra to create space before filling it with cement, helping restore spinal alignment.
- Vertebroplasty: Involves injecting cement directly into the fractured vertebra to stabilise and support the bone.
Both procedures are performed under local or general anaesthesia and typically take 30 minutes to an hour per vertebra.
Kyphoplasty & Vertebroplasty at St John & St Elizabeth Hospital
At St John & St Elizabeth Hospital, we offer advanced care for patients with spinal fractures. Our experienced and compassionate consultants will guide you through every step of the process, from diagnosis to recovery, providing personalised treatment tailored to your needs.
Why choose us for kyphoplasty or vertebroplasty?
- Specialist Spinal Surgeons: Our consultants are highly skilled in treating spinal fractures using minimally invasive techniques.
- Personalised Care: We create tailored treatment plans based on your condition and goals, helping you achieve effective relief and improved mobility.
- Modern Facilities: Our hospital is equipped with advanced imaging and surgical tools to ensure precise diagnosis and treatment.
- Accessible Location: Based in NW8, we serve patients from Hampstead (NW3), Kilburn (NW6), and across London.
We are committed to providing excellent care and supporting your recovery every step of the way.
Surgeons who perform Kyphoplasty and Vertebroplasty in London
How Much Does Private Kyphoplasty & Vertebroplasty Cost?
from £13,775*
The cost of private Kyphoplasty & Vertebroplasty starts from £13,775* at St John & St Elizabeth Hospital.
*The price shown is an estimated guide to the hospital charges associated with your treatment from admission to discharge. Your final cost may vary depending on your individual clinical needs, the procedure performed, any additional treatments required, the type of implant/prosthesis used (where applicable), and the length of stay. This guide price excludes consultation fees, diagnostic tests, and professional fees charged separately by your surgeon, anaesthetist, and any other specialists involved in your care.
|
Spinal vertebra fracture repair surgery (single level) |
£13,775* |
|---|---|
|
Spinal vertebra fracture repair surgery (two levels) |
£17,075* |
|
Spinal vertebra fracture repair surgery (more than two levels) |
£20,225* |
How to pay for your treatment
If you’re… paying for yourself
Did you know you don’t need private medical insurance to come to St John & St Elizabeth Hospital? As a self-pay patient, you can access safe, outstanding quality health care at times to suit you.
For scans and tests, as well as to see most consultants, you’ll still need to be referred by a medical professional like your GP, but as a self-pay patient, the process is more straightforward. You won’t need authorisation from an insurance provider, and you’ll have greater choice of consultant and appointment times.
If you’re… insured
St John & St Elizabeth Hospital is approved by all major medical insurance companies. If you have a personal private health insurance policy, or your company provide it for you, you can use it to pay for your care from your initial consultation through to treatment, surgery and aftercare such as physiotherapy. Not all private health insurance plans cover the same things. It’s very important to check exactly what you are covered for with your insurance provider.
Frequently Asked Questions About Kyphoplasty & Vertebroplasty
St John & St Elizabeth Hospital is located in St John’s Wood (NW8), a well-connected area of North West London. We are conveniently accessible for patients from Hampstead (NW3), Kilburn (NW6), and beyond.
By Tube:
- St John’s Wood station (Jubilee Line) is just a 5-minute walk from the hospital.
- Finchley Road (NW3) and Kilburn stations (NW6) on the Jubilee Line provide excellent connections.
By Bus:
- Wellington Road: Routes 13, 46, and 113 stop near St John’s Wood Underground Station, just a short walk from the hospital.
- Circus Road: Routes 46 and 187 stop close to the hospital’s Circus Road entrance.
- Abbey Road: Routes 139 and 189 stop near the junction where Grove End Road becomes Abbey Road, providing easy access.
Major Roads:
If you’re travelling from NW3 or NW6, major routes such as Finchley Road or Kilburn High Road offer a direct approach to the hospital.
The cost of private fractured spine surgery such as kyphoplasty & vertebroplasty depends on the type of surgery you have.
The cost of fractured spinal vertebra repair surgery (single level) is £13,775 at St John & St Elizabeth Hospital.
The cost of fractured spinal vertebra repair surgery (two levels) is £17,075 at St John & St Elizabeth Hospital.
The cost of fractured spinal vertebra repair surgery (more than two levels) is £20,225 at St John & St Elizabeth Hospital.
Before your procedure, you will have a consultation with one of our expert specialists to review your medical history and perform a physical examination. Imaging studies, such as X-rays or MRIs, may be used to evaluate the fractures in your vertebrae. You may be asked to stop taking blood thinners or other medications before the procedure. You will receive specific instructions about fasting and any other preparations required to ensure a safe and effective treatment.
Both procedures typically take 30 minutes to an hour per vertebra, depending on the complexity of the fracture.
The procedures are performed under anaesthesia, so you won’t feel pain during treatment. Some mild soreness may occur afterward but usually resolves within a few days.
Most patients can return to light activities within a day or two. Full recovery and resumption of normal activities typically occur within a few weeks.
After the procedure, you will be monitored for a short period to ensure there are no immediate complications. You may experience some soreness at the injection site, but pain relief from the fractured vertebra is often felt quickly. Most patients can return to their normal activities within a few days to a week, although you should avoid heavy lifting or strenuous activities for a while. You will be provided with post-procedure care instructions, including recommendations for pain management and follow-up care.
These procedures are ideal for patients with painful spinal compression fractures caused by osteoporosis, trauma, or certain cancers. Your consultant will assess your condition to determine the most suitable treatment.
Kyphoplasty and vertebroplasty are minimally invasive procedures used to treat vertebral fractures, often caused by osteoporosis or injury. In both procedures, special medical cement is injected into the fractured vertebra to stabilise it and relieve pain. Kyphoplasty involves using a balloon to create space within the vertebra before the cement is injected, whereas vertebroplasty involves directly injecting the cement. These procedures are recommended when other treatment options, like medications or physical therapy, haven’t provided sufficient relief.
Yes, kyphoplasty is considered safe for elderly patients, especially those with osteoporosis-related spinal fractures. It helps stabilise the spine and may also restore some height to the fractured vertebra. The minimally invasive nature of the procedure makes it well-suited for older patients with reduced bone density.
Both vertebroplasty and kyphoplasty are safe procedures with low complication rates, particularly when performed by skilled surgeons. Kyphoplasty may offer additional benefits for certain patients by restoring vertebral height and reducing spinal deformity. Our consultants will recommend the most appropriate option based on your specific condition and overall health.