Contact number: 020 7806 4060
What Are Spinal Injections?
Back pain injections deliver anti-inflammatory medication, provide pain relief, or deliver both directly into the affected area of the spine. As a targeted back pain treatment, they can help reduce inflammation, ease discomfort and improve day-to-day movement.
These injections are commonly used to treat:
- Sciatica Pain that radiates down the leg due to nerve compression in the lower back.
- Spinal stenosis Narrowing of the spinal canal, which can cause pain, tingling or weakness in the back and legs.
- Herniated discs Pain caused by a bulging or ruptured disc pressing on nearby nerves.
- Arthritis Inflammation in the small facet joints of the spine, leading to stiffness and ongoing discomfort.
Spinal injections may be used to help confirm the source of your pain, provide short- to medium-term pain relief, or form part of a wider back pain treatment plan. This may include physiotherapy, lifestyle advice or, in some cases, surgery.
Why choose us for spinal injections?
- Specialist Pain Management Team: Our experts have extensive experience in performing spinal injections to treat a variety of conditions.
- Personalised Care: We tailor treatment to your specific symptoms and recovery goals.
- Modern Facilities: Our hospital features advanced imaging technology for precise injection placement and effective results.
- Accessible Location: Conveniently based in NW8, we serve patients from Hampstead (NW3), Kilburn (NW6), and the wider London area.
We are dedicated to helping you manage pain and restore mobility through expert, patient-focused care.
Spinal Injections at St John & St Elizabeth Hospital
At St John & St Elizabeth Hospital, we offer back pain injections as part of our advanced pain management services. Our caring and experienced consultants work with you to create a personalised treatment plan, providing effective relief and improved quality of life.
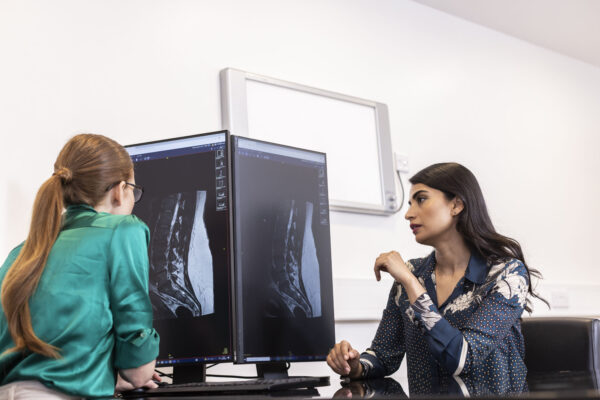
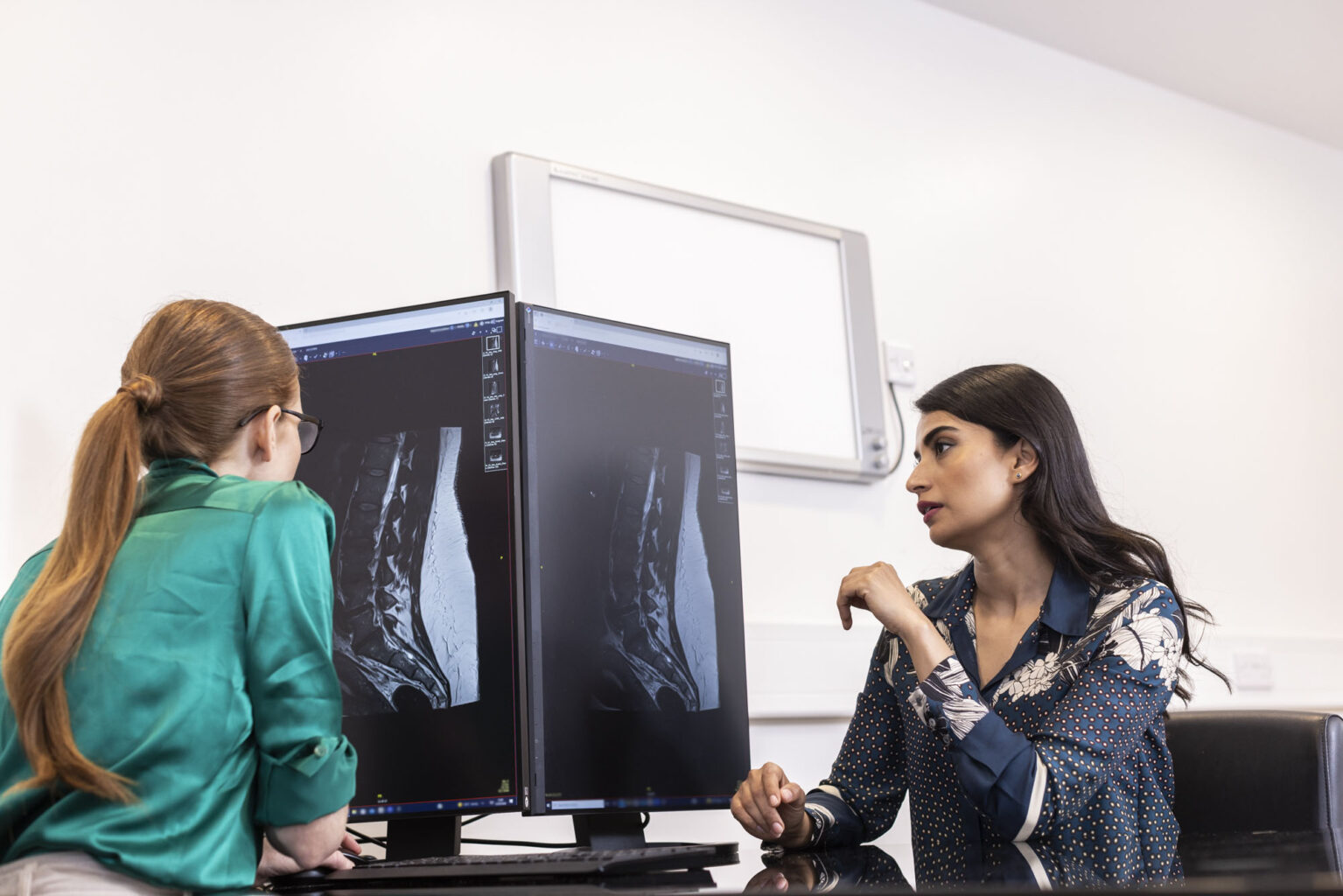
Medial branch block injections and image guidance
A medial branch block (MBB) is an image-guided spinal injection used to diagnose and manage pain coming from the facet joints in the spine. These joints can become inflamed due to arthritis or general wear and tear.
During the procedure, your consultant injects a local anaesthetic around the medial branch nerves, which carry pain signals from the facet joints. If your pain improves temporarily, it suggests these joints are the source of your symptoms.
Image guidance for accuracy and safety
We usually perform medial branch blocks under fluoroscopy (real-time X-ray). You will lie on your stomach on an X-ray table while your consultant carefully guides a fine needle into position. A small amount of contrast dye is used to confirm accurate placement before the medication is injected. In some cases, ultrasound may be used instead.
Image guidance helps ensure the injection is delivered precisely, improving diagnostic accuracy and reducing risk.
What to expect
The procedure takes around 20 to 30 minutes and is carried out as a same-day appointment. You should arrange for someone to drive you home and plan to rest for one to two days afterwards. Mild soreness at the injection site is common for a few days and can usually be managed with ice packs and simple pain relief.
Your consultant will talk you through the process and answer any questions before your appointment, so you feel informed and reassured.
Nerve Root Block with Image Guidance (including Bilateral Lumbar)
Nerve Root Block with Image Guidance, refers to a lumbar nerve root block procedure performed using imaging to guide the injection accurately. It involves injecting medication close to an inflamed nerve root in the lower spine to help relieve leg or lower back pain.
This outpatient procedure usually takes between 15 and 30 minutes. A local anaesthetic and steroid are injected near the affected nerve root to reduce inflammation and ease symptoms.
Image guidance and procedure steps
To ensure precise needle placement, the procedure is carried out under image guidance using a fluoroscope (X-ray) or CT scanner.
You will lie on your stomach while your consultant carefully positions the needle. A radiopaque contrast dye is used to confirm the needle is in the correct position before the medication is injected.
This procedure code also covers cases where treatment is required on both sides of the lumbar spine (bilateral injections).
Recovery and possible side effects
Patients usually go home the same day, but you will need someone to drive you home afterwards.
Some people may experience temporary numbness or weakness following the injection. There may also be a temporary increase in pain for a few days before symptoms begin to settle.
Your consultant will explain what to expect and provide guidance before and after your appointment.
Epidural Injection (Caudal)
Epidural Injection (Caudal) is used to treat chronic lower back and leg pain caused by inflamed nerves. The injection delivers a steroid and local anaesthetic into the epidural space through the sacral hiatus at the base of the spine.
Purpose and effectiveness
This injection aims to reduce swelling and inflammation around nerves in the lower spine. It may help relieve symptoms of sciatica, spinal stenosis and radiculopathy.
Some patients notice improvement within a few days, although the steroid can take up to two weeks to become fully effective. Pain relief can last from a few weeks to several months, and the procedure can be repeated if necessary.
Risks and recovery
After the injection, patients are generally advised to rest for 24 hours and avoid strenuous activity. Complications are rare but can include headache, infection, nerve damage or temporary numbness.
How the procedure is performed
The injection is usually carried out under sedation, although sometimes only a local anaesthetic is used. Imaging guidance, such as ultrasound or X-ray, is often used to ensure accurate needle placement.
Consultants who perform Spinal Injections in London
How to pay for your treatment
If you’re… paying for yourself
Did you know you don’t need private medical insurance to come to St John & St Elizabeth Hospital? As a self-pay patient, you can access safe, outstanding quality health care at times to suit you.
For scans and tests, as well as to see most consultants, you’ll still need to be referred by a medical professional like your GP, but as a self-pay patient, the process is more straightforward. You won’t need authorisation from an insurance provider, and you’ll have greater choice of consultant and appointment times.
If you’re… insured
St John & St Elizabeth Hospital is approved by all major medical insurance companies. If you have a personal private health insurance policy, or your company provide it for you, you can use it to pay for your care from your initial consultation through to treatment, surgery and aftercare such as physiotherapy. Not all private health insurance plans cover the same things. It’s very important to check exactly what you are covered for with your insurance provider.
Frequently Asked Questions About Spinal Injections
St John & St Elizabeth Hospital is located in St John’s Wood (NW8), a well-connected area of North West London. We are conveniently accessible for patients from Hampstead (NW3), Kilburn (NW6), and beyond.
By Tube:
- St John’s Wood station (Jubilee Line) is just a 5-minute walk from the hospital.
- Finchley Road (NW3) and Kilburn stations (NW6) on the Jubilee Line provide excellent connections.
By Bus:
- Wellington Road: Routes 13, 46 and 113 stop near St John’s Wood Underground Station, just a short walk from the hospital.
- Circus Road: Routes 46 and 187 stop close to the hospital’s Circus Road entrance.
- Abbey Road: Routes 139 and 189 stop near the junction where Grove End Road becomes Abbey Road, providing easy access.
Major Roads:
If you’re travelling from NW3 or NW6, major routes such as Finchley Road or Kilburn High Road offer a direct approach to the hospital.
- Epidural steroid injections. These help relieve pain in the back and in the areas near the spinal nerve roots. Sometimes, they can also be used to reduce arm or leg pain. They are often used to help manage pain caused by a herniated disc, spinal stenosis, or radiculopathy.
- Facet joint injections. The facet joints connect the bones of the spine. Nerve roots pass near these joints and connect the spinal cord to peripheral nerves. This injection works by injecting a mixture of local anaesthetic and steroid (an anti-inflammatory) into the facet joints in your spinal canal. It may be recommended if you suffer from arthritis or other conditions of the facet joints.
- Medial branch nerve blocks: This is a test to see if your neck and back pain is caused by your facet joints. In a medial branch block, your doctor will inject local anaesthetic over the nerves in your facet joint. If this relieves your pain, it will confirm the facet joints are the source of your pain.
- Radiofrequency ablation (aka radiofrequency denervation): This procedure involves putting a needle into the nerves by the facet joints in your back. Radiofrequency waves are then used to damage the nerves to reduce your pain.
- Sacroiliac joint injections: The sacrum is the large bony part at the base of the spine. This injection can be used to diagnose and treat certain types of lower back pain. A mixture of local anaesthetic and steroid is used, which will help reduce pain in the joint as well as tackle surrounding inflammation.
Before your spinal injection, you will have a consultation with one of our specialist consultants who will review your medical history, symptoms, and previous treatments. Imaging studies such as X-rays or MRIs may be used to identify the specific area causing the pain. You may be advised to stop taking certain medications, like blood thinners, before the procedure. Detailed pre-procedure instructions, including fasting and any other preparations, will be provided to ensure a safe and effective injection.
Spinal injections are typically recommended for conditions such as herniated discs, spinal stenosis, sciatica, or chronic back pain that hasn’t responded to other treatments like physical therapy or oral medication. The injections can provide pain relief, reduce inflammation, and promote healing in the affected area.
Spinal injections typically take 15 to 30 minutes, with additional time for preparation and observation afterward.
Most patients experience minimal discomfort during spinal injections. A local anaesthetic is used to numb the area, and the procedure is performed under imaging guidance for accuracy.
Recovery is usually quick, with many patients returning to normal activities the same or next day. Mild soreness at the injection site is normal but typically resolves within a day or two.
After the procedure, you may experience some soreness or temporary discomfort at the injection site, but this typically resolves within a few hours to a few days. Pain relief from the injection can start within a few days, and for some patients, the effects can last for weeks or even months. It’s important to follow post-procedure instructions, including any restrictions on physical activity, to promote healing and avoid complications. If you experience any severe pain or side effects, it’s important to contact your doctor immediately.
The duration of relief varies depending on the condition being treated and the type of injection. Some patients experience relief for several weeks to months, while others may require repeat injections as part of their treatment plan.
Yes, spinal steroid injections can be highly effective for many patients. They provide targeted relief from pain and inflammation caused by conditions such as sciatica, spinal stenosis, or herniated discs. While not a permanent solution, they can significantly improve mobility and quality of life, particularly when combined with physiotherapy or other treatments.
Yes, most patients can walk immediately after a spinal steroid injection. However, it’s recommended to rest and avoid strenuous activities for the first day to ensure the best results and minimise any potential soreness at the injection site.