Contact number: 020 7806 4060
What Is a Discectomy?
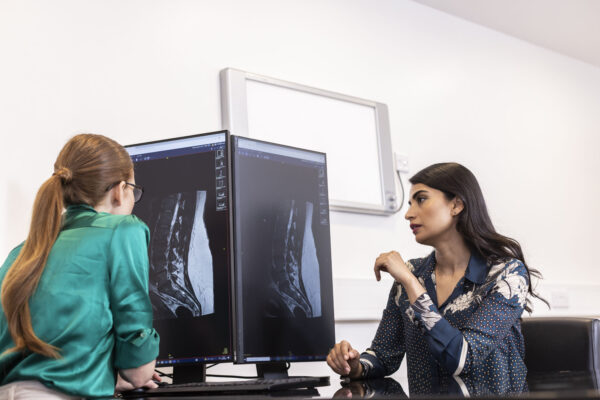
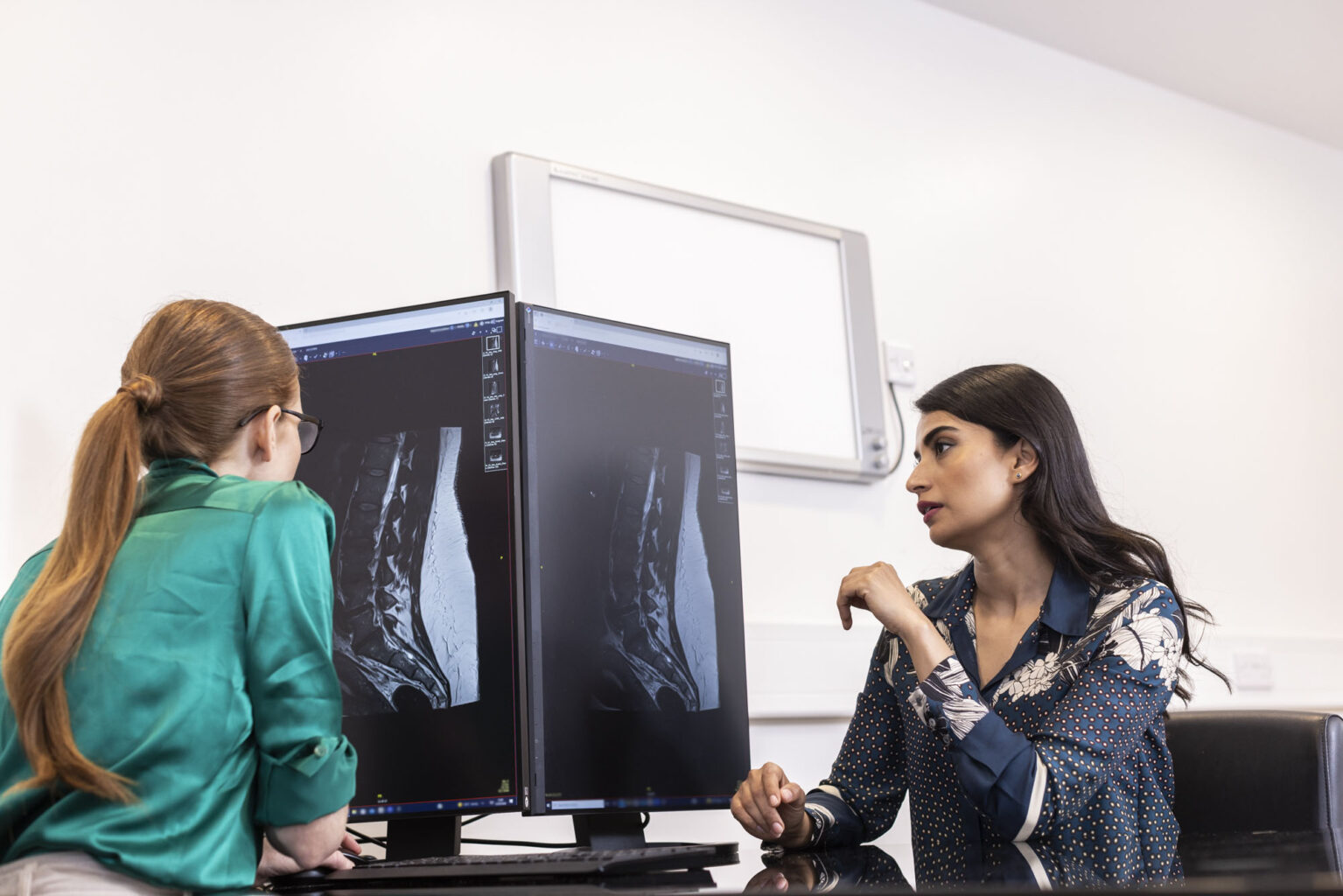
A discectomy involves the removal of part or all of a herniated disc in the spine. Herniated discs can press on nearby nerves, causing pain, numbness, or weakness, often in the back, legs, or arms. This procedure aims to relieve these symptoms by reducing nerve compression.
A discectomy is typically recommended for patients with:
- Persistent pain that doesn’t improve with non-surgical treatments like physiotherapy or medication
- Numbness or weakness affecting daily activities
- Severe sciatica or nerve-related pain in the arms or legs
Discectomy at St John & St Elizabeth Hospital
At St John & St Elizabeth Hospital, we offer discectomy surgery as part of our spinal care services. Our experienced and caring surgical team provides a personalised and thorough approach to your treatment, prioritising your recovery and long-term comfort.
Why choose us for discectomy surgery?
- Specialist Surgeons: Our consultants are highly experienced in spinal surgery, including discectomy procedures.
- Personalised Care: We create tailored treatment plans to address your specific symptoms and goals.
- Modern Facilities: Our hospital is equipped with advanced imaging and surgical tools for precise diagnosis and treatment.
- Accessible Location: Based in NW8, we serve patients from Hampstead (NW3), Kilburn (NW6), and across London.
We are dedicated to helping you find relief from back pain and supporting your journey to recovery.
Surgeons who perform Discectomy and Microdiscectomy in London
How Much Does Private Discectomy Surgery Cost?
from £9,325*
The cost of private Discectomy and Microdiscectomy starts from £9,325* at St John & St Elizabeth Hospital.
*The price shown is an estimated guide to the hospital charges associated with your treatment from admission to discharge. Your final cost may vary depending on your individual clinical needs, the procedure performed, any additional treatments required, the type of implant/prosthesis used (where applicable), and the length of stay. This guide price excludes consultation fees, diagnostic tests, and professional fees charged separately by your surgeon, anaesthetist, and any other specialists involved in your care.
How to pay for your treatment
If you’re… paying for yourself
Did you know you don’t need private medical insurance to come to St John & St Elizabeth Hospital? As a self-pay patient, you can access safe, outstanding quality health care at times to suit you.
For scans and tests, as well as to see most consultants, you’ll still need to be referred by a medical professional like your GP, but as a self-pay patient, the process is more straightforward. You won’t need authorisation from an insurance provider, and you’ll have greater choice of consultant and appointment times.
If you’re… insured
St John & St Elizabeth Hospital is approved by all major medical insurance companies. If you have a personal private health insurance policy, or your company provide it for you, you can use it to pay for your care from your initial consultation through to treatment, surgery and aftercare such as physiotherapy. Not all private health insurance plans cover the same things. It’s very important to check exactly what you are covered for with your insurance provider.
Frequently Asked Questions About Discectomy Surgery
St John & St Elizabeth Hospital is located in St John’s Wood (NW8), a well-connected area of North West London. We are conveniently accessible for patients from Hampstead (NW3), Kilburn (NW6), and beyond.
By Tube:
- St John’s Wood station (Jubilee Line) is just a 5-minute walk from the hospital.
- Finchley Road (NW3) and Kilburn stations (NW6) on the Jubilee Line provide excellent connections.
By Bus:
- Wellington Road: Routes 13, 46, and 113 stop near St John’s Wood Underground Station, just a short walk from the hospital.
- Circus Road: Routes 46 and 187 stop close to the hospital’s Circus Road entrance.
- Abbey Road: Routes 139 and 189 stop near the junction where Grove End Road becomes Abbey Road, providing easy access.
Major Roads:
If you’re travelling from NW3 or NW6, major routes such as Finchley Road or Kilburn High Road offer a direct approach to the hospital
A discectomy typically takes 1 to 2 hours, depending on the complexity of the condition and the surgical approach used.
The procedure is performed under general anaesthesia, so you won’t feel pain during surgery. Mild discomfort may occur during recovery but is manageable with medication and rest.
Before your surgery, you will meet with one of our spinal consultants, who will assess your condition, take your medical history, and potentially recommend scans such as X-rays or MRIs to identify the location and severity of the problem. If surgery is recommended, your doctor will explain the potential risks, benefits, and details of the procedure. Preparation for surgery includes pre-operative tests, possibly an MRSA test, and specific instructions regarding medications such as blood thinners. You will also be advised to refrain from eating or drinking for a certain period before surgery.
On the day of your surgery, wear loose, comfortable clothing and bring a small bag with essentials such as toiletries, your phone, charger, medications, and a change of clothes. Once admitted, a nurse will check your vital signs and review your medical history. Your doctor will go over the procedure one last time before you sign the consent form, and you will be prepared for surgery.
During the procedure, you will be given general anaesthesia and will remain asleep throughout. The surgeon will make an incision along your spine, exposing the affected disc. Using an X-ray to guide them, they will remove the necessary disc tissue or bone to relieve pressure on the nerves, leaving most of the disc in place to maintain its shock-absorbing function. The surgery typically takes 60 to 90 minutes, after which you will be monitored in the recovery area.
After surgery, you will be moved to your private room to begin recovery. You will start physical therapy the day after your operation to help you regain mobility. Depending on your condition, you may stay in the hospital for one to several days. Your stitches may be dissolvable or require removal in about 10 days. You will also be given instructions for aftercare, including a post-operative check with your surgeon. It is normal to feel sore for a few weeks, and your recovery could take up to six weeks.
Most patients can return to light activities within a few weeks. Full recovery, including returning to work and physical activities, may take 6 to 8 weeks, depending on your condition and recovery progress.
To promote healing, it’s important to follow your surgeon’s advice and adhere to your physiotherapy program. Gradually increase your activity levels, avoid sitting or standing in one position for too long, and take care of your incision site. You may need help at home during the first week. Most people need around 6 weeks off work, but if your job is physically demanding, you might need 8-12 weeks. If needed, ask for a ‘fitness to work’ certificate before you leave the hospital.
Yes, discectomy surgery is often highly effective in relieving pain, numbness, and weakness caused by herniated discs, allowing patients to regain mobility and improve their quality of life.
A discectomy is generally considered a moderately invasive surgery rather than a major one. While it requires general anaesthesia and careful precision, it is typically performed as a routine procedure with a relatively short recovery period for most patients.
Most patients stay in the hospital for 1 to 2 days after a discectomy. Some procedures, particularly minimally invasive ones, may even be performed as day cases, allowing patients to go home the same day.
Discectomy is considered a low-risk surgery when performed by experienced surgeons, like our caring surgeons at St John St Elizabeth Hospital. Like all surgeries, it carries some risks, such as infection or nerve damage, but complications are rare, and most patients recover without issues.
The results of a discectomy can last for many years, with most patients experiencing long-term relief from pain and other symptoms. Regular follow-ups and a healthy lifestyle can help maintain the benefits.